Aldosterone breakthrough in dogs with naturally occurring myxomatous mitral valve disease

Author information
Ames MK, Atkins CE, Eriksson A, Hess AM. Aldosterone breakthrough in dogs with naturally occurring myxomatous mitral valve disease // J Vet Cardiol. 2017 Jun;19(3):218-227.
Abstract
INTRODUCTION: Aldosterone breakthrough (ABT) is the condition in which angiotensin converting enzyme inhibitors (ACEIs) and/or angiotensin receptor blockers fail to effectively suppress the activity of the renin angiotensin aldosterone system. The objective of this study was to determine if ABT occurs in dogs with naturally occurring myxomatous mitral valve disease receiving an ACEI, using the urine aldosterone to creatinine ratio (UAldo:C) as a measure of renin angiotensin aldosterone system activation.
ANIMALS, MATERIALS AND METHODS: This study includes 39 dogs with myxomatous mitral valve disease. A UAldo:C cut-off definition (derived from a normal population of healthy, adult, and client-owned dogs) was used to determine the prevalence of ABT in this population. Spearman analysis and univariate logistic regression were used to evaluate the relationship between UAldo:C and ABT (yes/no) and eight variables (age, serum K+ concentration, serum creatinine concentration, ACEI therapy duration and ACEI dosage, furosemide therapy duration and furosemide dosage, and urine sample storage time). Finally, the UAldo:C in dogs receiving spironolactone, as part congestive heart failure (CHF) therapy, was compared to dogs with CHF that were not receiving spironolactone.
RESULTS: The prevalence of ABT was 32% in dogs with CHF and 30% in dogs without CHF. There was no relationship between either the UAldo:C or the likelihood of ABT and the eight variables. Therapy with spironolactone lead to a significant elevation of the UAldo:C.
DISCUSSION: Using the UAldo:C and a relatively stringent definition of ABT, it appears that incomplete RAAS blockade is common in dogswith MMVD receiving an ACEI. The prevalence of ABT in this canine population mirrors that reported in humans. While the mechanism of ABT is likely multifactorial and still poorly understood, the proven existence of ABT in dogs offers the potential to improve the prognosis for MMVD with the addition of a mineralocorticoid receptor blocker to current therapeutic regimens.
CONCLUSIONS: Approximately 30% of dogs being treated for heart disease and CHF satisfied the definition of ABT. Identifying patient subpopulations experiencing ABT may help guide future study design and clinical decision-making.
KEYWORDS: Angiotensin converting enzyme inhibitor; Heart failure; Mineralocorticoid receptor blocker; Renin angiotensin aldosterone system
Abbreviations
- i>ABT aldosterone breakthrough<
- ACE angiotensin converting enzyme
- ACEI angiotensin converting enzyme inhibitor
- ARB angiotensin 1-receptor blocker
- CHF congestive heart failure
- MMVD myxomatous mitral valve disease
- MRB mineralocorticoid receptor blockade/blocker
- RAAS renin angiotensin aldosterone system
- RIA radioimmunoassay
- UAldo:C urine aldosterone to creatinine ratio
Chronic activation of the sympathetic nervous system and renin angiotensin aldosterone system (RAAS) results in sodium and water retention, vasoconstriction (increased preload and afterload), and cardiovascular remodeling. This neurohormonal activation promotes and perpetuates the congestive heart failure (CHF) syndrome. Plasma renin activity and blood concentrations of aldosterone and norepinephrine, which increase as heart disease progresses, are markers and contributors to the hemodynamic derangements of this syndrome [1—5]. Importantly, loop- diuretic therapy, and sodium restriction further stimulate RAAS activation [5—7].
Improved understanding of the pathological consequences of neurohormonal activation has led to beneficial heart failure therapies beyond loop diuretics in veterinary medicine, most notably angiotensin converting enzyme inhibitors (ACEIs) [8—11]. Furthermore, benefits seen with inodilating drugs, such as pimobendan, are likely due, in part, to reduced circulating neurohormone levels produced by improvements in hepatic and renal perfusion, more efficient metabolism and excretion of these compounds, and reduced stimuli for their release. However, despite improved CHF pharmacotherapy, morbidity, and mortality remain high.
When secreted chronically and in excess, aldosterone has been implicated in the increased generation of reactive oxygen species, inflammation, and pathologic remodeling (hypertrophy and fibrosis) in tissues such as myocardium, vascular smooth muscle, and kidneys [12—15]. Aldosterone levels have been found to be increased in people with chronic and acutely decompensated CHF [2,3,6]. It had been presumed that both ACEI and angiotensin 1-receptor blockers (ARB) would effectively blunt aldosterone secretion by reducing the formation of angiotensin II (a major secretagogue of aldosterone). It is now known that angiotensin converting enzyme inhibitors and ARB (alone or in combination) do not always effectively suppress aldosterone secretion in people and this phenomenon is referred to as aldosterone breakthrough (ABT) [16—25]. In humans, ABT is an important, well-accepted, yet poorly understood phenomenon, in those treated with ACEI or ARB for chronic kidney disease, heart failure, and hypertension [16,20,21,25,26].
Despite its acceptance, there is no consensus regarding ABT’s exact definition, timing, and prevalence. Creating a definition of aldosterone breakthrough requires a reliable screening tool to evaluate aldosterone levels. As previously described by the authors, the urine aldosterone to creatinine ratio (UAldo:C), using spot urine samples, can be used as a surrogate for 24-h urinary aldosterone excretion, allowing assessment of RAAS activity in dogs [27]. Using the UAldo:C, the authors have demonstrated ABT in normal research dogs where, despite angiotensin converting enzyme inhibitors therapy, aldosterone levels rise duringrenin angiotensin aldosterone system activation with either a diuretic or vasodilator [27—30].
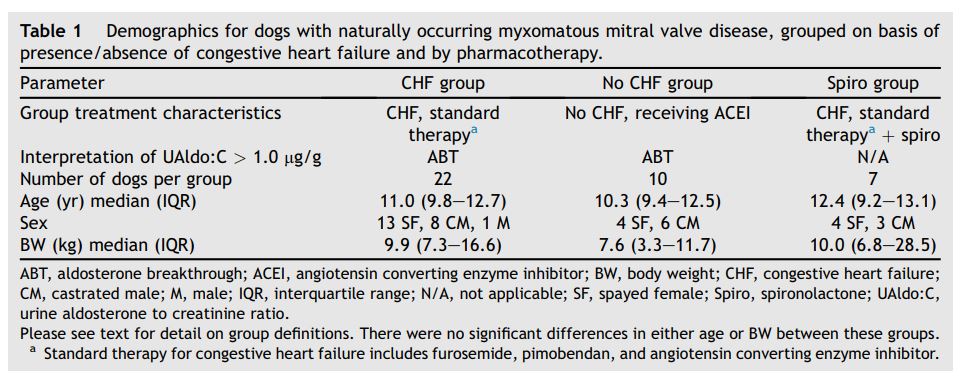
Table 1 Demographics for dogs with naturally occurring myxomatous mitral valve disease, grouped on basis of presence/absence of congestive heart failure and by pharmacotherapy.
Plasma angiotensin converting enzyme (ACE) activity was measured in three of these studies and was found to decrease significantly within 1 day of oral angiotensin converting enzyme inhibitors administration [27], yet the incidence of ABT in these studies was found to be as high as 60%. Although these experiments involved normal dogs in subacute studies, they raised the question as to whether aldosterone breakthrough occurs in dogs with naturally occurring heart disease.
Myxomatous mitral valve disease (MMVD) is the most common acquired cardiovascular disease and the most common cause of CHF in dogs. Angiotensin converting enzyme inhibitor are indicated once a patient is in CHF (American College of Veterinary Internal Medicine [ACVIM] stage C), yet it remains controversial as to whether they confer benefit, prior to the onset of CHF (ACVIM stage B1 and B2) [31].
Identification of subpopulations of dogs with MMVD, experiencing ABT, may help guide future study design and clinical decision-making. The goal of this study was to use the UAldo:C to determine both the existence and frequency of ABT in dogs with naturally occurring MMVD. This study also sought to investigate the mechanism of aldosterone breakthrough by evaluating the relationships between UAl- do:C and ABT (yes/no) and eight variables (age, serum K+ concentration, serum creatinine concentration, ACEI therapy duration and dosage, furosemide therapy duration and dosage, and urine sample storage time). The first seven variables were chosen, as they are hypothesized to play a role in the mechanisms of aldosterone breakthrough. The variable 'sample storage time’ was chosen to determine if duration of sample freezing affects aldosterone concentration. Finally, the UAldo:C from dogs receiving spironolactone as part of CHF therapy was compared to that of dogs with CHF, not receiving spironolactone.
Materials and methods
Animals
Dogs with MMVD that presented to the cardiology and emergency services of the North Carolina State University College of Veterinary Medicine and Colorado State University College of Veterinary Medicine and Biomedical Sciences were enrolled into this study between 6/2012 and 6/ 2014. In this study, CHF was defined as the presence of cardiogenic pulmonary edema, necessitating furosemide administration.
A board certified cardiologist (MA or CA) confirmed the diagnosis of MMVD and of CHF, when present. Dogs already receiving therapy for MMVD were prospectively placed into three groups, based on the presence/absence of a proven history of CHF and their pharmacotherapy (Table 1). Dogs with MMVD and CHF receiving 'standard therapy’ (furosemide, pimobendan, and angiotensin converting enzyme inhibitors) were included in the CHF group. An ACEI (enalapril or benazepril) was required to have been used for greater than one day for dogs to be enrolled in the study. Dogs with MMVD and CHF, receiving 'standard therapy’ (ACEI, furosemide, and pimobendan) and spironolactone, were included in the Spiro group. Dogs with MMVD without CHF, that were receiving an ACEI, were placed in the no CHF group. The authors prospectively collected the data from all recruited and enrolled dogs, and then allocated them to their respective treatment groups. The investigators did not impose treatment regimens, rather accepted or rejected cases from the study, based in part on their therapies. Concurrent medications (cardiac and non-cardiac), other than angiotensin 1-receptor blockers, were allowed. Dogs with controlled systemic hypertension or endocrine disease were permitted. Patients were excluded if they did not fit the criteria of one of the three groups or if their urine sample was not handled per the study protocol. The Institutional Animal Care and Use Committees approved this study at both institutions.
Urine aldosterone to creatinine ratio (UAldo:C)
About 2—5 mL of a free-catch urine sample was collected from each dog, immediately refrigerated and then frozen at -70 C, within 24 h of collection. Samples were submitted for determination of UAldo:C. If blood work was deemed necessary by the primary clinician, as part of the dog’s medical and treatment plan, then a sample was taken for serum biochemical analysis. The blood samples were taken on the same day as the urine collection and were obtained via venipuncture (jugular, cephalic, or saphenous) with the dog gently restrained in a sitting or lateral position. The timing of urine collection was not standardized for these clinical patients, presenting at various times of the day to both the cardiology and emergency services. A radioimmunoassay (RIA) that has been validated in dogsc was used to measure urine aldosterone concentration. Urine creatinine concentration was measured via a standard colorimetric assay. For all samples, these two components of the UAldo:C were performed by a veterinary diagnostic laboratory.01 The same RIA assay was used for all analyses and the assay performed per the manufacturer’s directions, as described elsewhere [28]. Briefly, this assay measures free aldosterone and one of its two major metabolites, aldosterone b-glucuronide (after acid hydrolysis to aldosterone).
Definition of aldosterone breakthrough
The normal (baseline) UAldo:C has been studied (using an RIAc to measure urine aldosterone) in 34 healthy, <6-year-old laboratory dogs (mean UAl- do:C of 0.40 ± 0.21 mg/g) and 21 client-owned, normal, >5-year-old dogs (mean UAldo:C of 0.49 mg/g, ± 0.27).e Only 1 of these 55 dogs (a dog in the <6-year-old group) had a UAldo:C greater than 1.0 mg/g. From these historical data, it appears that the UAldo:C usually does not exceed 1.0 mg/g, and the UAldo:C does not appear to change significantly with age in normal dogs. The mean + 2 SD of the UAldo:C of the older dogs from Colorado State University was 1.0 mg/g and this value was used to determine our cut-off definition for ABT (UAldo:C > 1.0 ug/g).
Statistical analysis
The D’Agostino—Pearson omnibus procedure was used to test for normality. Data are presented as median and interquartile range (median; IQR). There were 32 dogs receiving an angiotensin converting enzyme inhibitors without spironolactone (CHF, no CHF groups) included in the analysis for ABT. The occurrence of ABT is presented as a percentage. The Spearman test was used to evaluate the relationship between UAldo:C ratio vs. eight variables (age, serum K+ concentration, serum creatinine concentration, ACEI therapy duration and dosage, furosemide therapy duration and dosage, and urine sample storage time). All 32 dogs receiving an ACEI were included in this analysis. Sample storage time was defined as the time from collection to analysis. Univariate logistic regression was used to look at the relationship between aldosterone breakthrough (yes/no, using the definition of UAldo:C > 1.0 mg/g) and each of the eight variables above for those same 32 dogs. The Benja- mini—Hochberg procedure was used to adjust p- values for multiple testing.
The mean age, body weight, UAldo:C, and ACEI dosages and durations were compared between the three groups (CHF, no CHF, and Spiro) using the Kruskal—Wallace test with Dunn’s adjustment for multiple comparisons. The Mann—Whitney U test was used to compare the furosemide dosages and durations between the CHF and Spiro groups. The Mann—Whiney U test was also used to compare ACEI type (enalapril vs. benazepril) and UAldo:C for dogs in the CHF and no CHF groups. The Fisher’s exact test was used to determine if there was a relationship between ABT and presence of CHF. The criteria for statistical significance was set to a = 0.05. Analyses were performed using the e Ames MK, Atkins CE, Webb K. The urine aldosterone to creatinine ratio (UALDO:C) determined by radioimmunoassay (RIA) in normal dogs greater than 5 years of age. J Vet Intern Med 2015; 29: 1148 (abstract).
Results
Animals
Forty-one dogs were enrolled into this study and 39 dogs were included, as they fit the criteria for one of the groups described in Table 1. Twenty-nine of these 39 dogs had a serum biochemistry performed on the same day as their urine sample collection. The CHF group was made up of 22 dogs with both acute (<2 weeks of furosemide therapy; n = 10) and chronic (>2 weeks of furosemide therapy; n = 12) CHF. The no CHF group was made up of 10 dogs, all but one of which was placed in ACVIM stage B2 MMVD. One dog, in stage B1 MMVD, was on amlodipine and an ACEI as chronic therapy for systemic hypertension. There were seven dogs in the Spiro group. There were no differences in age or body weight between the three groups (p=0.64 and p=0.28, respectively).
ACEI, furosemide, and spironolactone: dosage and duration
The number of dogs receiving each type of angiotensin converting enzyme inhibitors (enalapril or benazepril) in the CHF, and no CHF groups and the average dosages are shown in Fig. 1. The median (IQR) durations of ACEI administration for dogs in the CHF, no CHF, and Spiro groups were 86 (12—233), 297 (15—713), and 787 (164—1,661) days, respectively. Three of the 39 (7.7%) had been receiving an angiotensin converting enzyme inhibitors for less than one week. There were no differences in ACEI dosages between the three groups (p=0.8).
The median (IQR) dosages of furosemide for dogs in the CHF and Spiro groups were 3.7 (1.8—4.2) and 3.4 (1.9—6.7) mg/kg/day and the median (IQR) durations of furosemide administration were 28 (7—110) and 229 (91—792) days, respectively. Both the mean dosage and duration of furosemide therapy were significantly greater in the Spiro group (p=0.0001 and p=0.02, respectively). Within the CHF group, 6 dogs had received furosemide for <2 weeks and 16 dogs had received furosemide for >2 weeks. Dogs in the Spiro group received a dosage of spironolactone (median [IQR]) of 1.7 (1.0—1.8) mg/kg/day receiving spironolactone had received it for more than one week. All dogs f SAS, version 9.4, SAS Institute Inc, Cary, North Carolina, USA. g GraphPad Prism v6.0 La Jolla, CA, USA.
Figure 1 Angiotensin converting enzyme inhibitor (ACEI) type and dosage shown as a scatter dot plot (median and interquartile range) in dogs with myxomatous mitral valve disease (MMVD).
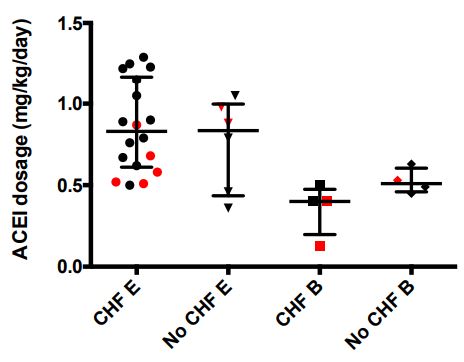
CHF B, 4 dogs with congestive heart failure (CHF), receiving benazepril as part of standard CHF therapy (ACEI, furosemide, and pimobendan); CHF E, 18 dogs with CHF, receiving enalapril, as part of standard CHF therapy; no CHF B, 4 dogs with MMVD, without CHF, receiving benazepril; no CHF E, 6 dogs with MMVD, without CHF, receiving enalapril. There were no significant differences between these groups. Red dots indicate dogs with UAldo:C > 1.0 mg/g (aldosterone breakthrough).
Urine aldosterone to creatinine ratio
Urine samples from the 39 dogs were submitted for analysis of UAldo:C. The majority of samples were collected between the hours of 9 am and 5 pm. The UAldo:C results from the three groups are shown in Fig. 2. The median (IQR) UAldo:C results in the Spiro group were 2.3 (1.3—5.7) mg/g. None of the eight variables (age, serum K+ concentration, serum creatinine concentration, angiotensin converting enzyme inhibitors duration and dosage, furosemide duration and dosage, and urine sample storage time) were significantly correlated with UAldo:C (p-values all > 0.49). The UAldo:C for dogs with MMVD receiving spironolactone (Spiro group; n = 7) was significantly greater than that for dogs with MMVD and CHF, not receiving spironolactone (CHF group, p<0.05) and dogs with MMVD, not in CHF (no CHF group, p<0.05). There was no difference in UAl- do:C between the CHF and no CHF groups (p>0.05).
ABT and renin angiotensin aldosterone system activation
The percentages of ABT in the CHF and no CHF groups were 32% and 30% respectively (Table 2 and Fig. 2). Within the CHF group, the percentage of ABT in dogs with subacute (<2 weeks of furosemide therapy) and chronic (>2 weeks of furosemide therapy) CHF was 50% and 25%, respectively.
Figure 2 Urine aldosterone to creatinine ratio (UAl- do:C) as a scatter dot plot (median and interquartile range) in dogs with myxomatous mitral valve disease (MMVD), with and without congestive heart failure (CHF).
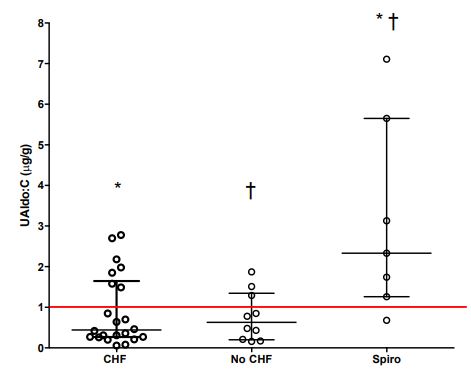
Dogs receiving spironolactone (Spiro), in addition to standard therapy (furosemide, pimobendan, and an ACEI), demonstrated significantly higher UAldo:C than dogs in the other groups. Individual dogs experiencing aldosterone breakthrough (ABT) were 7 of 22 (CHF group, receiving standard therapy) and 3 of 10 (no CHF group, receiving ACEI). Six of 7 dogs in the Spiro group (receiving standard therapy plus spironolactone) had a UAldo:C > 1.0 mg/g. Red line denotes upper limit of normal UAldo:C (>1.0 mg/g).
Based on univariate regression analysis, none of the eight variables (age, serum K+ concentration, serum creatinine concentration, angiotensin converting enzyme inhibitors duration and dosage, furosemide duration and dosage, and urine sample storage time) were predictive of ABT (p-values all >0.63). Similarly, in the CHF and no CHF groups, when the enalapril dosage was compared between dogs with ABT and those without ABT, there was no difference (p=0.23, Fig. 3).
Discussion
From these results, it appears that aldosterone breakthrough is a common occurrence in dogs with naturally occurring MMVD, being treated with ACEI. Aldosterone break through occurred in 32% in dogs with CHF and 30% in dogs that were not yet in CHF. The definition of ABT used in this study is stringent, as compared to human medical definitions of ABT, which often only require that the value of blood aldosterone be either greater than the mean of a normal population, greater than the upper limit of a reference interval for a normal population, or greater than an individual’s baseline value. Overall, it appears that approximately 30% of dogs in this study had inadequate renin angiotensin aldosterone system blockade.
No correlation was found between ACEI dosage and therapy duration and either the UAldo:C or the presence of aldosterone breakthrough. In regards to angiotensin converting enzyme inhibitors dosage, the results of this study are similar to those of small studies in people with CHF [22] and dogs with experimental RAAS activation [28], which have not shown that higher dosages of ACEI prevent ABT. It is, however, noteworthy that, although there were dogs receiving enalapril at dosages of less than 0.5mg/kg/day that did not experience aldosterone breakthrough, no dog receiving enalapril at a dosage greater than 1mg/ kg/day experienced ABT (Fig. 3). The relationship between duration of ACEI therapy and ABT has not been well studied in either man or dog. The dogs in this study had been receiving an ACEI for varying durations, including three dogs in the CHF and no CHF groups that had received less than one week’s therapy. Of interest, 1 of 3 dogs (33%) demonstrated ABT, a percentage similar to that of dogs MMVD stage is based on the ACVIM consensus statement. A single dog with controlled systemic hypertension and stage B1 MMVD receiving and ACEI was included. Please see text for detail on group definitions receiving chronic therapy.
Table 2 The mean UAldo:C for each myxomatous mitral valve disease group is presented with the incidence of aldosterone breakthrough.
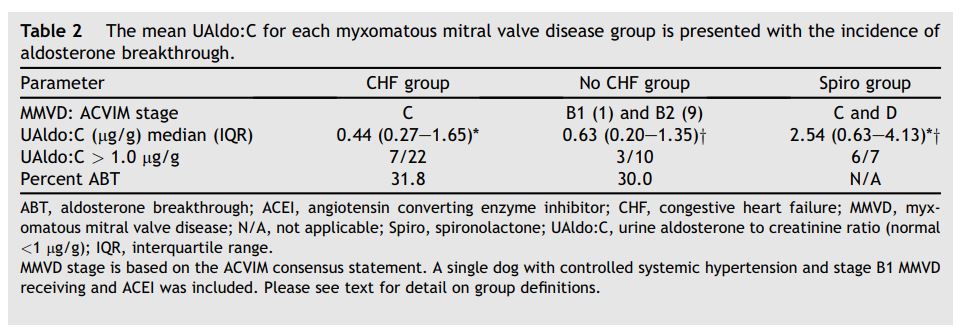

Figure 3 Scatter dot plot (median and interquartile range) of angiotensin converting enzyme inhibitor (enalapril) dosage and aldosterone breakthrough (ABT) status in 24 dogs receiving enalapril for the management of myxomatous mitral valvular disease with (CHF group) and without (no CHF group) congestive heart failure.
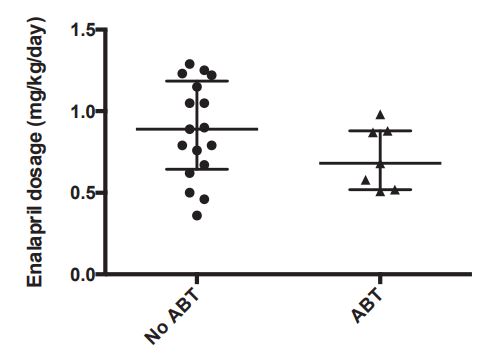
None of these 24 dogs received spironolactone. The dogs are divided into 2 groups—those that experienced aldosterone breakthrough (ABT) and those that did not (no ABT). These enalapril dosages were not significantly different.
As it may take weeks for the maximal beneficial effects of ACEI to be realized [32,33], elevated urinary aldosterone levels during the first month of therapy may be temporary. It can be argued, however, that incomplete RAAS blockade for the first weeks/months of therapy is suboptimal, and that its recognition may be clinically useful. There does not appear to be a relationship between the presence of ABT and the presence of CHF. Additionally, aldosterone breakthrough may occur both before and after the onset of CHF. Finally, there was no correlation between either UAldo:C or the presence of ABT and age, serum K+ concentration, serum creatinine concentration, duration and dosage of furosemide therapy, or urine sample storage time.
Once spironolactone is administered, the UAl- do:C is difficult to interpret as blockade of the mineralocorticoid receptor leads to an increase in circulating and urine aldosterone concentrations, presumably due to receptor occupation and the failure of an aldosterone-generated negative feedback loop to lower renin secretion from the juxtaglomerular apparatus [34]. The consequences of high levels of free, circulating aldosterone are still unknown in such patients, but the miner- alocorticoid receptor-mediated effects of aldosterone are inhibited [35,36]. The non—receptor- mediated effects of aldosterone, however, remain under investigation. Based on the mortality benefit attributed to spironolactone in people with heart failure and low ejection fraction [37—39] and in dogs with MMVD [40] that are treated with spironolactone, the pathophysiologic impact of high levels of aldosterone with concurrent miner- alocorticoid receptor blockade, do not appear to negatively impact outcome on a population basis. The study presented here was designed to prove the existence and determine the rate of occurrence of aldosterone breakthrough in canine veterinary patients, but not designed to evaluate the impact of ABT on survival. However, the aforementioned study in dogs with heart failure due to MMVD has already demonstrated a survival benefit, when mineralocorti- coid receptor blockade/blocker (MRB) was added to standard heart failure therapy (including an angiotensin converting enzyme inhibitors) [40].
There is no consensus regarding the definition of ABT in people, and clinical definitions are usually based on spot blood aldosterone concentrations, using either a baseline definition (a patient’s blood aldosterone concentration increases despite ACEI/ ARB therapy) or a cut-off definition (while receiving an ACEI/ARB, a patient’s blood aldosterone concentration is greater than the mean or mean + 2 standard deviations of a normal population). A baseline definition can be used when pre-treatment samples are available, allowing 'individualization’ and monitoring of 'anti-RAAS’ therapy in a way that is independent of the aldosterone assay used. A cut-off definition is the only option; however, when baseline data are unavailable (i.e. the patient is already on ACEI or angiotensin 1-receptor blockers therapy). Furthermore, while controversy exists regarding the use of ACEI in MMVD prior to the onset of CHF, pre-treatment assessment of UAldo:C, would help to clarify the potential benefit of anti-RAAS therapy at this stage. In human CHF patients, treatment with the MRBs, spironolactone and eplerenone, is associated with an improved prognosis, on a population basis. The mechanism is thought to be through combatting ABT [37—39].
Increased aldosterone levels in heart disease/ failure results not only from increased secretion (RAAS stimulation) but also through decreased neurohormone metabolism and clearance (due to decreased hepatic and renal perfusion) [41,42]. Circulating ACE activity is reduced by label dosages of the ACEI, benazepril, and enalapril, in both healthy dogs receiving furosemide as a renin angiotensin aldosterone system stimulant, and in dogs with naturally occurring MMVD and CHF [29,30,43,44]. As ABT has been documented to occur despite the reduction in ACE activity that attends ACEI administration, mechanisms other than failure of ACE-inhibition likely occur. Non—ACE-dependent pathways for angiotensin II production, other stimuli for aldosterone release, and decreased aldosterone metabolism and clearance have all been hypothesized as mechanisms for ABT [16,18]. Along with angiotensin II, blood potassium concentration is a key regulator of aldosterone secretion [13]. An elevated potassium concentration, secondary to angiotensin converting enzyme inhibitors or other cause, may contribute to ABT. This role of this hypothesis in aldosterone breakthrough in the studied population, however, is not supported by our data. Another possible mechanism for ABT is the excessive production of renin, associated with the use of ACEI, wherein excess renin secretion 'overwhelms’ the actions of the ACEI, allowing aldosterone production [18]. In none of the dogs, described herein, was plasma renin concentration measured and it is therefore unknown if renin upregulation contributed to the observed ABT. Three additional possibilities for ABT in clinical patients may be related to the therapy of heart failure. The first is potentiation of renin angiotensin aldosterone system activation by diuretics, salt restriction, and vasodilators, which are commonly used in the pharmacotherapy of heart failure [44—47]. Second, activation of the sympathetic nervous system with heart failure may be potentiated by the use of certain cardiac medications, as has been documented with the administration of amlodipine in humans with systemic hypertension [48]. Finally, compliance is a major problem in patients, both human and animal, and might be expected to worsen with length of time under treatment, due to cost, patient or owner fatigue, and drug side-effects. Failure to take/give the ACEI would be associated with angiotensin converting enzyme inhibitors 'failing’ to suppress aldosterone, mimicking breakthrough. These proposed explanations are not mutually exclusive.
This study has several limitations related to its small sample size. First, it was not designed to evaluate survival and there is only minimal evidence that ABT influences survival in dogs with naturally occurring heart disease.h There is, however, evidence supporting an influence of elevated aldosterone levels and/or ABT on cardiorenal outcomes in people [49,50]. An antecedent study in dogs, however, has shown that an MRB (spironolactone), added to ACEI in dogs with MMVD, confers an added benefit in survival [40]. This historical study, along with the present study, supports the existence and importance of ABT in dogs and suggest a potential benefit with additional RAAS blockade in the form of an MRB. Second, a firm conclusion cannot be made regarding correlation between the UAldo:C or ABT and the eight variables studied herein. Therefore, the mechanism(s) of aldosterone breakthrough remain unknown. Additionally, the absence of measurement of renin angiotensin aldosterone system hormonal elements, other than ACE activity and UAldo:C, make answering some mechanistic questions impossible.
Despite these limitations, our results show that aldosterone breakthrough occurs in approximately 30% of dogs receiving an angiotensin converting enzyme inhibitors for MMVD, mirroring the findings in humans with cardiovascular disease, and those in our experimental model of ABT. The mechanism of ABT is likely multifactorial and variable between individuals. Further study should be undertaken to determine if ABT is correlated to worsened prognosis, to evaluate its permanence and consistency in a given patient, and to elucidate its mecha- nism(s). Finally, a priori identification of patient subpopulations experiencing or expected to experience aldosterone breakthrough may help guide future study design and clinical decision-making, as whether to initiate MRB therapy in an individual patient.
References
- Swedberg K, Eneroth P, Kjekshus J, Wilhelmsen L. Hormones regulating cardiovascular function in patients with severe congestive heart failure and their relation to mortality. CONSENSUS Trial Study Group. Circulation 1990;82: 1730—6.
- Anker SD, Chua TP, Ponikowski P, Harrington D, Swan JW, Kox WJ, Poole-Wilson PA, Coats A. Hormonal changes and catabolic/anabolic imbalance in chronic heart failure and their importance for cardiac cachexia. Circulation 1997; 96:526—34.
- Broqvist M, Dahlstrom U, Karlberg BE, Karlsson E, Marklund T. Neuroendocrine response in acute heart failure and the influence of treatment. Eur Heart J 1989;10: 1075—83.
- Levine TB, Francis GS, Goldsmith SR, Simon AB, Cohn JN. Activity of the sympathetic nervous system and renin- angiotensin system assessed by plasma hormone levels and their relation to hemodynamic abnormalities in congestive heart failure. Am J Cardiol 1982;49:1659-66.
- Francis GS, Benedict C, Johnstone DE, Kirlin PC, Nicklas J, Liang C, Kubo SH, Rudin-Toretsky MS,Yusuf S. Comparison of neuroendocrine activation in patients with left ventricular dysfunction with and without congestive heart failure. Circulation 1990;82:1724-9.
- Aronson D, Burger AJ. Neurohormonal prediction of mortality following admission for decompensated heart failure. Am J Cardiol 2003;91:245-8.
- Bayliss J, Norell M, Canepa-Anson R, Sutton G, Poole- Wilson P. Untreated heart failure: clinical and neuroendocrine effects of introducing diuretics. Br Heart J 1987; 57:17-22.
- The COVE Study Group. Controlled clinical evaluation of enalapril in dogs with heart failure: results of the Cooperative Veterinary Enalapril Study Group. J Vet Intern Med 1995;9:243-52.
- The BENCH BENazepril in Canine Heart Disease Study Group. The effect of benazepril on survival times and clinical signs of dogs with congestive heart failure: results of a multi-center, prospective, randomized, double- blinded, placebo-controlled, long-term clinical trial. J Vet Cardiol 1999;1:7-18.
- Ettinger S, Benitz A, Ericsson G, Cifelli S, Jernigan A, Longhofer S, Trimboli W, Hanson PD. Effects of enalapril maleate on survival of dogs with naturally occurring acquired heart failure. J Am Vet Med Assoc 1998;213:1573-7.
- AmbergerC, Chetboul V, Bomassi E, Rougier S, Woehrle F, Thoulon F. Comparison of the effects of imidapril and enalapril in a prospective, multicentric randomized trial in dogs with naturally acquired heart failure. J Vet Cardiol 2004;6:9-16.
- Gilbert KC, Brown NJ. Aldosterone and inflammation. Curr Opin Endocrinol Diabetes Obes 2010;17:199-204.
- Waanders F, de Vries LV, van Goor H, Hillebrands J-L, Laverman GD, Bakker SJL, Navis G. Aldosterone, from (patho)physiology to treatment in cardiovascular and renal damage. Curr Vasc Pharmacol 2011;9:594-605.
- Young M, Fullerton M, Dilley R, Funder JW. Mineralocorti- coids, hypertension, and cardiac fibrosis. J Clin Investig 1994;93:2578-83.
- Schiffrin EL. Effects of aldosterone on the vasculature. Hypertension 2006;47:312-8.
- Bomback AS, Klemmer PJ. The incidence and implications of aldosterone breakthrough. Nat Clin Pract Nephrol 2007; 3:486-92.
- Cicoira M, Zanolla L, Rossi A, Golia G, Franceschini L, Cabrini G, Bonizzato A, Graziani M, Anker SD, Andrew JS, Coats DM, Zardini P. Failure of aldosterone suppression despite angiotensin-converting enzyme (ACE)inhibitor administration in chronic heart failure is associated with ACE DD genotype. J Am Coll Cardiol 2001;37:1808-12.
- Sato A. Aldosterone breakthrough during angiotensinconverting enzyme inhibitor therapy. Am J Hypertens 2003;16:781-8.
- Sato A, Saruta T. Aldosterone escape during angiotensinconverting enzyme inhibitor therapy in essential hypertensive patients with left ventricular hypertrophy. J Intern Med 2001;29:13-21.
- Lee A, MacFadyen RJ. Neurohormonal reactivation in heart failure patients on chronic ACE inhibitor therapy: a longitudinal study. Eur J Heart Fail 1999;1:401-6.
- MacFadyen RJ, Lee AFC, Morton JJ, Pringle SD, Struthers AD. How often are angiotensin II and aldosterone concentrations raised during chronic ACE inhibitor treatment in cardiac failure? Heart 1999;82:57-61.
- Tang WHW, Vagelos RH, Yee Y-G, Benedict C, Wilson K, Liss C, LaBelle P, Fowler MB. Neurohormonal and clinical responses to high- versus low-dose enalapril therapy in chronic heart failure. J Am Coll Cardiol 2002;39:70-8.
- Schjoedt KJ, Andersen S, Rossing P, Tarnow L, Parving H-H. Aldosterone escape during blockade of the renin- angiotensin-aldosterone system in diabetic nephropathy is associated with enhanced decline in glomerular filtration rate. Diabetologia 2004;47:1936-9.
- Horita Y, Taura K, Taguchi T, Furusu A, Kohno S. Aldosterone breakthrough during therapy with angiotensinconverting enzyme inhibitors and angiotensin II receptor blockers in proteinuric patients with immunoglobulin A nephropathy. Nephrology 2006;11:462-6.
- Bomback AS, Rekhtman Y, Klemmer PJ, Canetta PA, Radhakrishnan J, Appel GB. Aldosterone breakthrough during aliskiren, valsartan, and combination (aliskiren + valsartan) therapy. J Am Soc Hypertens 2012; 6:338-45.
- Soberman JE, Weber KT. Spironolactone in congestive heart failure. Curr Hypertens Rep 2000;2:451-6.
- Ames MK, Atkins CE, Lantis AC, Brunnen zum J. Evaluation of subacute change in RAAS activity (as indicated by urinary aldosterone: creatinine, after pharmacologic provocation) and the response to ACE inhibition. J Renin Angiotensin Aldosterone Syst 2016;17:1-12.
- Ames MK, Atkins CE, Lee S. Effects of high doses of ena- lapril and benazepril on the pharmacologically activated renin-angiotensin-aldosterone system in clinically normal dogs. Am J Vet Res 2015;76:1041-50.
- Lantis AC, Ames MK, Atkins CE, DeFrancesco TC, Keene BW, Werre SR. Aldosterone breakthrough with benazepril in furosemide-activated renin-angiotensin- aldosterone system in normal dogs. J Vet Pharmacol Ther 2014;38:65-73.
- Lantis AC, Ames MK, Werre S, Atkins CE. The effect of enalapril on furosemide-activated renin-angiotensin- aldosterone system in healthy dogs. J Vet Pharmacol Ther 2015;38:513-7.
- Atkins C, Bonagura J, Ettinger S, Fox P, Gordon S, Haggstrom J, Hamlin R, Keene B, Luis-Fuentes V, Stepien R. Guidelines for the diagnosis and treatment of canine chronic valvular heart disease. J Vet Intern Med 2009;23:1142-50.
- Gansevoort RT, de Zeeuw D, de Jong PE. Dissociation between the course of the hemodynamic and antiproteinuric effects of angiotensin I converting enzyme inhibition. Kidney Int 1993;44:579-84.
- Gansevoort RT, de Zeeuw D, de Jong PE. Is the antiproteinuric effect of ACE inhibition mediated by interference in the renin-angiotensin system? Kidney Int 1994;45: 861 -7.
- Briet M, Schiffrin EL. Vascular actions of aldosterone. J Vasc Res 2013;50:89-99.
- Vinson GP, Coghlan JP. Expanding view of aldosterone action, with an emphasis on rapid action. Clin Exp Pharmacol Physiol 2010;37:410-6.
- Gekle M, Grossmann C. Actions of aldosterone in the cardiovascular system: the good, the bad, and the ugly? Pflugers Arch Eur J Physiol 2008;458:231-46.
- Pitt B, Zannad F, Remme WJ, Cody R, Castigne A, Perez A, Palensky J, Wittes J. The effect of spironolactone on morbidity and mortality in patients with severe heart failure. N Engl J Med 1999;341:709-17.
- Pitt B, Remme W, Zannad F, Neaton J, Martinez FA, Roniker B, bittman R, Hurley S, Kleiman J, Gatlin M. Eplerenone, a selective aldosterone blocker, in patients with left ventricular dysfunction after myocardial infarction. N Engl J Med 2003;348:1309-21.
- Zannad F, McMurray J, Krum H, van Veldhuisen DJ, Swedberg K, Shi H, Vincent J, Pocock SJ, Pitt B. Epler- enone in patients with systolic heart failure and mild symptoms. N Engl J Med 2011;364:11-21.
- Bernay F, Bland JM, Haggstrom J, Baduel L, Combes B, Lopez A, Kaltsatos V. Efficacy of spironolactone on survival in dogs with naturally occurring mitral regurgitation caused by myxomatous mitral valve disease. J Vet Intern Med 2010;24:331-41.
- Schneider EG, Davis JO, Baumber JS, Johnson JA. Renin, aldosterone, and hypertension. The hepatic metabolism of renin and aldosterone. A review with new observations on the hepatic clearance of renin. Circ Res 1970;27:175-83.
- Coppage Jr WS, Island DP, Cooner AE. The metabolism of aldosterone in normal subjects and in patients with hepatic cirrhosis. J Clin Investig 1962;41:1672-80.
- Toutain PL, Lefebvre HP, King JN. Benazeprilat disposition and effect in dogs revisited with a pharmacokinetic/ pharmacodynamic modeling approach. J Pharmacol Exp Ther 2000;292:1087-93.
- Haggstrom J, Hansson K, Karlberg BE, Kvart C, Madej A, Olsson K. Effects of long-term treatment with enalapril or hydralazine on the renin-angiotensin-aldosterone system and fluid balance in dogs with naturally acquired mitral valve regurgitation. Am J Vet Res 1996;57:1645-52.
- Atkins CE, Rausch WP, Gardner SY, DeFrancesco TC, Keene BW, Levine JF. The effect of amlodipine and the combination of amlodipine and enalapril on the renin- angiotensin-aldosterone system in the dog. J Vet Pharmacol Ther 2007;30:394-400.
- Lantis AC, Atkins CE, DeFrancesco TC. Effects of furo- semide and the combination of furosemide and the labeled dosage of pimobendan on the circulating renin- angiotensin-aldosterone system in clinically normal dogs. Am J Vet Res 2011;72:1646-51.
- Lovern CS, Swecker WS, Lee JC, Moon ML. Additive effects of a sodium chloride restricted diet and furosemide administration in healthy dogs. Am J Vet Res 2001;62: 1793-6.
- Champlain J de, Karas M, Assouline L, Nadeau R, LeBlanc AR, Dube B, Larochelle P. Effects of valsartan or amlodipine alone or in combination on plasma catecholamine levels at rest and during standing in hypertensive patients. J Clin Hypertens 2007;9:168-78.
- Deo R, Yang W, Khan AM, Bansal N, Zhang X. Serum aldosterone and death, end-stage renal disease, and cardiovascular events in blacks and whites. Hypertension 2014;64:103-10.
- Girerd N, Pang PS, Swedberg K, Fought A, Kwasny MJ, Subacius H, Konstam MA, Maggioni A, Gheorghiade M, Zannad F. Serum aldosterone is associated with mortality and re-hospitalization in patients with reduced ejection fraction hospitalized for acute heart failure: analysis from the EVEREST trial. Eur J Heart Fail 2014;15:1228-35.
^Наверх









